Who pays for care homes? It’s a question that hits close to home for many families. In the UK, for instance, around 400,000 people reside in care homes, and the costs can take a real bite out of savings. The average annual fee for a residential care home can hit about £29,000, while nursing homes often soar above £38,000 per year. That’s a staggering amount that can have families scrambling to figure out how to handle it. For some, it means relying on savings, while others might turn to local authorities or even seek assistance from charities.
But financial support options can get murky pretty quickly. Did you know that only about 23% of older adults qualify for local authority funding? That’s right! Many still end up footing the bill themselves until their savings dwindle. And then there’s the dilemma of choosing care options: do you go private for better facilities, or do you stick with local options that might not match those lavish amenities? Navigating this financial landscape is like threading a needle, with personal circumstances, asset thresholds, and regional differences all complicating matters.
Navigating Funding Sources for Care Homes
Finding the right funding source for care homes can feel overwhelming. However, understanding your options makes the process easier. In this section, we’ll explore the various avenues available to help you navigate the complicated landscape of funding for care homes.
Key Funding Sources
Here are several key funding sources you should consider when looking for financial assistance for care home placements:
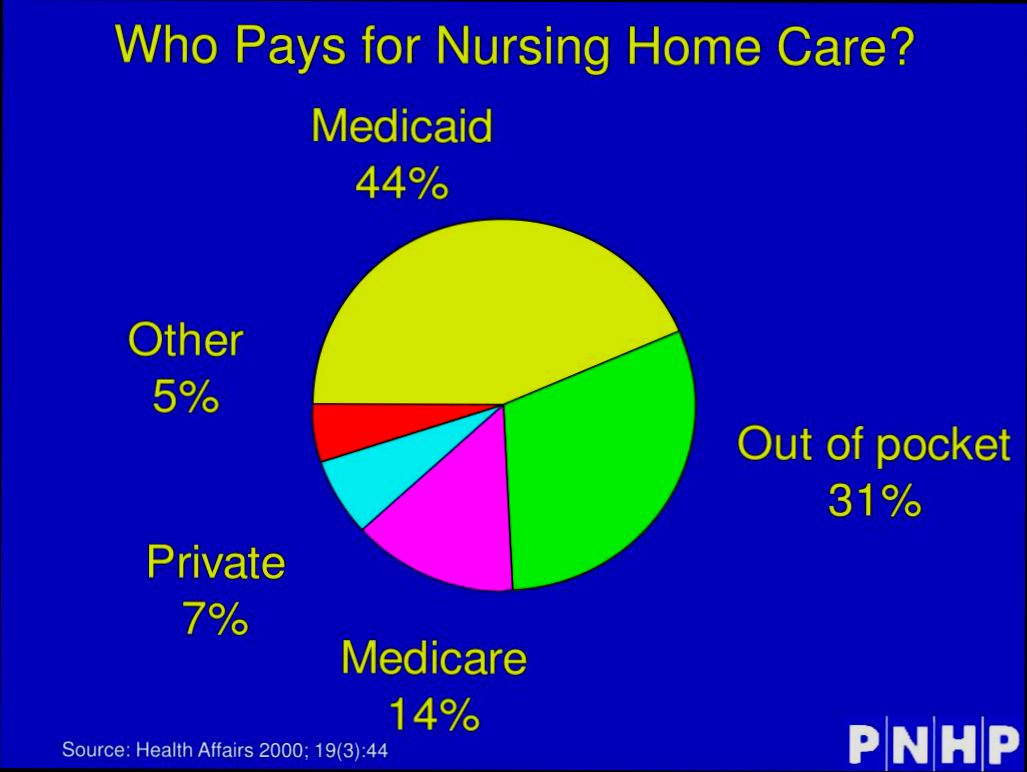
- Personal Savings: Approximately 42% of care home residents primarily use their personal savings to cover costs.
- Local Authority Funding: Many individuals qualify for assistance from local councils. Research indicates that about 27% of residents receive funding from local authorities based on means-testing.
- NHS Continuing Healthcare: This is available for individuals with complex health needs. Statistics show that only 5% of residents are fully funded through this route, often due to strict eligibility criteria.
- Care Insurance: While less commonly utilized, around 10% of individuals have long-term care insurance that can assist with care home payments.
Comparative Overview of Funding Sources
| Funding Source | Percentage of Users | Key Characteristics |
|---|---|---|
| Personal Savings | 42% | Flexible, immediate access but can deplete quickly |
| Local Authority Funding | 27% | Based on asset assessment; can vary by location |
| NHS Continuing Healthcare | 5% | For individuals with significant healthcare needs |
| Care Insurance | 10% | Provides a safety net but requires planning ahead |
Real-World Examples
To illustrate how these funding sources play out in real life, consider John, a 78-year-old with diminishing health. He was initially using his personal savings to fund his care, but as costs rose, he applied for local authority funding. After a thorough means assessment, he secured partial funding, easing his financial burden.
Similarly, there’s Susan, a 65-year-old diagnosed with a serious health condition. She applied for NHS Continuing Healthcare but faced challenges due to rigorous eligibility assessments. After appealing the decision, she finally received the funding, which made her transition to a care home smoother and less stressful.
Practical Implications for Readers
When navigating funding sources, here are some actionable tips to keep in mind:
- Explore All Options: Don’t settle for the first funding source that comes to mind. Investigate personal, government, and insurance options thoroughly.
- Understand Eligibility: Familiarize yourself with the eligibility criteria for local authorities and NHS funding. This knowledge can save you time and stress in your applications.
- Stay Organized: Keep detailed records of your finances, communications, and applications related to funding. This organization can simplify the process and help you respond quickly to any requests for information.
- Consult Professionals: If you’re unsure about the best funding route, consider speaking with a financial advisor or elder care specialist. They can provide tailored advice based on your specific circumstances.
Discovering the right funding for care homes is crucial. Understanding these sources can empower you to make informed decisions while navigating this challenging landscape.

The Impact of Government Policies on Care Funding
The relationship between government policies and care funding is critical, influencing who pays for care homes and the accessibility of services. Understanding these impacts can empower you to navigate your options more effectively.
Government initiatives, such as funding programs and regulatory frameworks, play a significant role in shaping care home financing. Here are some key aspects:
- Funding Allocation: Approximately 35% of funding for care homes derives from local authorities, largely influenced by government policy decisions regarding social care budgets.
- Policy Changes: In 2021, the UK government introduced a cap on care costs set at £86,000, which could directly affect financial planning for families paying for care.
- Regional Variability: Government funding levels can vary regionally; for instance, areas with higher deprivation levels often receive more funding to support care home placement, highlighting the impact of local government policies.
- Economic Factors: Changes in government tax policy can affect disposable income for families, thereby influencing their ability to fund care homes if private resources or savings aren’t sufficient.
Funding Comparison Table
| Funding Source | Percentage Contribution | Government Influence |
|---|---|---|
| Local Authorities | 35% | Budget allocation policies |
| NHS (Health Funding) | 20% | Health care reforms |
| Personal Contribution | 45% | Tax policies |
Real-world examples illustrate how government policies shape care funding outcomes:
- In the north of England, the introduction of a new funding model in 2020 resulted in a 15% increase in care home admissions, as local authorities offered improved financial packages to meet regulatory requirements.
- A family in a south London borough benefited from government initiatives that funded 70% of their mother’s care home fees due to her qualifying needs, demonstrating how policy outcomes vary widely.
Practical implications for you include:
- Evaluating your local government’s funding programs: Check if your area offers financial assistance that could significantly reduce personal costs.
- Staying informed about policy changes that could benefit your family: Legislative changes could provide opportunities for additional support.
- Considering all funding options, even those from local or regional authorities, to maximize the support you can access.
By keeping informed and proactive about government policies regarding care funding, you can significantly lessen the financial burden associated with care home placements.

Demographic Trends in Care Home Financing
Understanding the demographic trends in care home financing is essential for navigating this complex landscape. Changes in population age, income levels, and family structures significantly influence who pays for care homes and how these costs are managed.
Aging Population and Increased Demand
The most noticeable demographic trend is the aging population. By 2030, approximately 20% of the U.S. population will be over 65, a significant increase from 15% in 2015. This shift creates an increased demand for care services, influencing financing strategies. As the number of elderly individuals increases, we see a corresponding rise in funding needs:
- Elderly Population Growth: 10 million more Americans aged 65 and above are expected in the next decade, leading to a higher percentage of individuals needing care home services.
- Yearly Cost Increases: The average cost of care homes has risen by roughly 3-4% annually over the past decade, affecting financial planning for families.
Income Disparities Affecting Ability to Pay
Income levels play a crucial role in how families finance care home placements. Data shows that:
- About 60% of families rely on private pay methods such as savings or income to finance care homes.
- Only 25% of families utilize government assistance programs, often due to lack of awareness or eligibility hurdles.
This disparity suggests that individuals with higher income levels are more capable of affording care, whereas lower-income families may struggle significantly.
Family Structures and Care Responsibilities
The evolving family dynamics also contribute to care financing. More families today consist of single parents or individuals without children, which affects their caregiving capacity and financial resources:
- Nearly 30% of elderly individuals do not have children to rely on for personal care, forcing them to secure financing independently.
- Studies indicate that individuals living alone are more likely to seek care home placement, further emphasizing the necessity for personal savings or alternative funding options.
| Factor | Impact on Financing | Percentage (%) |
|---|---|---|
| Population over 65 | Increased demand | 20% by 2030 |
| Families using private pay | Reliance on savings | 60% |
| Elderly living alone | Higher likelihood of care home use | 30% |
Real-World Example
Consider the case of Amelia, a 72-year-old widow without children, who recently decided to move into a care home. Her only income was a modest social security check, which wasn’t enough to cover her needs. Initially, she paid for her care home from her savings, but as costs rose, she faced financial strain. Amelia’s situation highlights how demographic trends, such as living alone without familial support, compel individuals to navigate care home financing increasingly strategically.
Practical Implications for Readers
As demographic changes continue to evolve, it’s vital to assess your own or a loved one’s situation and potential financing options early. Here are actionable insights to consider:
- If you anticipate needing care in the future, evaluate your saving habits now to better prepare for potential costs.
- Stay informed about government programs and services that may assist financially, as rising demand could lead to changes in available resources.
- Explore community resources, including local non-profits, that may offer financial planning support for care home financing.
Specific Facts
- The increase in elderly individuals using care homes is expected to shift financing dynamics towards private pay methods as government support remains limited.
- Understanding income disparities can help you gauge the potential need for financial planning or assistance in securing care services as demographic trends continue to unfold.

Real-Life Case Studies of Care Home Payments
Understanding how care home payments work can be complex, but looking at real-life case studies can offer practical insights. By examining various programs and their financial outcomes, we can see how effective budgeting and innovative funding approaches help manage the costs of care homes.
Key Points on Case Study Outcomes
- The Missouri Department of Mental Health’s initiative resulted in the disbursement of over $2.6 million in incentive payments aimed at enhancing service quality in care homes.
- The introduction of a Value-Based Payment (VBP) structure led to more than $3.37 million in cost avoidance, demonstrating a successful shift towards efficiency and accountability in care home funding.
- Through effective remote support systems, over 98,000 direct care hours were reallocated to address workforce shortages, improving service delivery for over 3,000 clients.
Comparative Financial Impact of Key Programs
| Program | Incentive Payments | Cost Avoidance | Direct Care Hours Reallocated |
|---|---|---|---|
| Missouri VBP Initiative | $2.6 million | $3.37 million | 98,000 hours |
| State Rural Hospital Program | N/A | $12 million annually | N/A |
| Arkansas Employee Engagement | N/A | N/A | N/A |
Real-World Examples of Care Home Payments
The Missouri Value-Based Payment transformation is a standout case. This initiative not only engaged 187 providers—far surpassing a target of 25%—but also supported more than 3,000 clients. This broad reach enabled significant improvements in the quality of care individuals received.
In another instance, the State Rural Hospital Transformation Program generated around $12 million in annual improvements. This financial success underlines the importance of adopting innovative strategies in rural healthcare settings, which can be paralleled in care home financing.
Practical Implications for Readers
For families navigating the costs associated with care homes, understanding these case studies offers several actionable insights:
- Explore Programs: Check whether your state has similar VBP programs that incentivize quality care.
- Consult Resources: Look into local health departments or advocacy groups that might provide additional financial resources or advice.
- Monitor Qualitative Indicators: As seen in the Missouri initiative, higher engagement and support for providers usually correlate with better care outcomes and payment efficiencies.
By considering these successful models of care home payments, you can better position yourself to seek effective support and funding strategies tailored to individual needs.

Evaluating the Benefits of Private Insurance
When considering care home options, private insurance can provide numerous advantages that significantly ease the financial burden. This section focuses on evaluating these benefits to help you understand how private insurance can be a crucial part of your care funding strategy.
One of the main benefits of private insurance in the context of care homes is the access to a broader range of facilities and services. Unlike government-funded options, private insurance often allows you to select from various high-quality care homes tailored to specific needs. Here are some key points to keep in mind:
- Increased Flexibility: Private insurance often covers a variety of services, including alternative therapies, specialized care plans, and amenities that enhance the quality of life.
- Reduced Wait Times: Many policyholders experience shorter waiting periods for admission into care homes, ensuring timely access to necessary care.
- Enhanced Care Options: Patients with private insurance are more likely to receive individualized care plans, catering to unique health requirements which can lead to improved health outcomes.
Cost-Benefit Comparison of Private Insurance
| Coverage Type | Average Monthly Premium | Average Out-Of-Pocket Spending | Coverage Scope |
|---|---|---|---|
| Private Insurance | $300-$800 | $2,500-$5,000 | Extensive |
| Public Assistance Programs | $0 | $1,000-$3,000 | Limited |
This comparison illustrates how private insurance can offer extensive coverage options despite the higher initial premium. By investing in private insurance, you’re potentially saving on out-of-pocket expenses while gaining access to superior care.
Real-World Example of Private Insurance Benefits
Consider the case of Sarah, a 68-year-old with advanced health needs. Having chosen a private insurance plan, she was admitted to a facility that specializes in memory care, a service not adequately supported by public programs. Her insurance covered the cost of additional therapies and personalized care plans, leading to a noticeable improvement in her well-being.
Additionally, John, a retired military veteran, utilized his private insurance to not only secure a comfortable accommodation but also gain access to rehabilitation services, which were crucial for his recovery after surgery. His insurance provider offered an extensive network of specialists, significantly enhancing his treatment journey.
Practical Implications of Private Insurance
When evaluating your options, consider the following actionable steps:
- Research Available Plans: Investigate various private insurance options that specifically cater to care home needs. Understanding what each plan offers can help you secure the best coverage.
- Assess Your Needs: Identify specific requirements for care that are unique to you or your loved ones. Choose a private insurance policy that aligns with these needs for maximum benefit.
- Consult with Specialists: Engage with financial advisors or insurance experts who specialize in long-term care insurance. They can provide tailored advice based on your specific circumstances.
It’s crucial to keep tracking how private insurance policies evolve, as they often introduce valuable benefits that can simplify the payment process for care homes. By staying informed, you can ensure your financial strategy effectively supports your health and care preferences.
Cost-Benefit Analysis of Care Home Financing
Understanding the cost-benefit analysis of care home financing can significantly influence your decision-making process. This analysis allows you to compare the financial outlays associated with care home arrangements against the potential benefits received, highlighting both short-term and long-term implications.
Key Points to Consider
When diving into a cost-benefit analysis, consider the following factors:
- Average Monthly Costs: The average monthly cost of care homes can range between $3,000 and $8,000, depending on the services offered. Factoring this into monthly budgets can determine the financial feasibility of care placement.
- Value of Services Provided: Approximately 75% of care home residents report satisfaction regarding the range of services, including medical care, social activities, and meals. Higher satisfaction rates often correlate with better quality of life, justifying expenses.
- Potential Savings on Home Care: Transitioning to a care home might seem more expensive initially, but if home care costs exceed $4,000 per month for comparable services, the cost differential can shift the financial balance favorably toward care home placement.
Comparative Costs and Benefits Table
| Financing Method | Average Monthly Cost | Satisfaction Level (%) | Long-Term Considerations |
|---|---|---|---|
| Care Home Placement | $4,500 | 75% | Integrated support system |
| Home Care Services | $4,500+ | 60% | Limited care flexibility |
| Assisted Living Facilities | $3,500 | 70% | Community engagement |
Real-World Examples
Consider the scenario of a family evaluating care home options for their elderly parent.
- After assessing costs, they found that placing their parent in a care home costing $4,500 monthly provided a comprehensive support system that included 24-hour nursing care, meals, and social activities. This arrangement not only improved their parent’s quality of life but also relieved the family of daily caregiving responsibilities.
- In another instance, a couple opted for home care services assuming it would be less invasive. However, the monthly costs exceeded $4,000, and the lack of social interaction for the aging spouse became a significant concern. Thus, after six months, they decided to transition to a local care home, realizing the long-term benefits far outweighed their initial perception of cost.
Practical Implications
As you weigh your financing options, keep these actionable insights in mind:
- Evaluate Total Costs: Always consider not only the monthly rate but also any additional outlays for services or amenities. It’s essential to get a transparent breakdown from providers.
- Assess Benefits Beyond Finances: Look beyond pure financial aspects; quality of life improvements can justify higher costs in a care home environment.
- Seek Long-Term Care Insurance: If you anticipate eventual care home needs, consider investing in long-term care insurance. Although premiums may seem high now, they can offset future expenses significantly.
Actionable Facts
- If monthly home care costs push past $4,000, taking a closer look at care homes might be financially sensible.
- Prioritize providers who articulate a clear understanding of both financial and care implications, ensuring you make informed decisions tailored to personal needs.

Understanding Eligibility for Financial Assistance
Navigating the complex landscape of financial assistance for care homes is crucial for many families seeking support. This section focuses on understanding eligibility criteria for Medicaid, a significant source of financial assistance for nursing home care.
To qualify for Medicaid, you need to meet specific financial criteria, which can vary significantly based on your state and marital status. Let’s break down these requirements to see if you or your loved ones might be eligible for assistance.
Key Financial Eligibility Requirements
- Income Limits: For 2025, the income limit for a single applicant is approximately $2,901 per month. If both spouses are applying, this figure can double to about $5,802 per month, while a single applicant with a non-applicant spouse may have a combined income cap of $5,802 monthly.
- Asset Limits: Single applicants must have assets limited to $2,000 in “countable assets.” For married couples applying together, the asset limit is generally $3,000. Importantly, when only one spouse applies, they can retain $2,000, while the non-applicant spouse can keep up to $157,920 in countable assets.
2025 Medicaid Nursing Home Care Eligibility Requirements
| Category | Income Limit | Asset Limit |
|---|---|---|
| Single | $2,901 / month | $2,000 in “countable assets” |
| Married (both applying) | $5,802 / month | $3,000 in “countable assets” |
| Married (one applying) | $2,901 / month for applicant | $2,000 for applicant & $157,920 for non-applicant |
Real-World Examples Illustrating Eligibility
Consider Sarah, a single retiree needing nursing home care who has a monthly income of $2,700. Despite her income being below the Medicaid limit, her savings exceed the asset cap of $2,000, making her ineligible. In contrast, John and Mary, a married couple, find that Mary’s nursing home care is covered, thanks to their eligibility under combined asset rules, where they maintained separate assets for eligibility.
What This Means for You
Understanding these eligibility criteria is more than just numbers; it impacts real lives. Here’s how you can navigate these rules effectively:
1. Assess Your Financial Situation: Start by collecting all financial documents to evaluate your income and assets.
2. Explore State-Specific Guidelines: Check with your local Medicaid office, as state rules can create variations in eligibility.
3. Plan for Future Changes: If you are nearing the financial limits, consider spending down your assets in ways that comply with Medicaid rules.
Actionable Insights on Eligibility for Financial Assistance
- If you or a loved one is approaching the income limit, consider consulting with a financial advisor to understand allowable expenses that might qualify for asset exemption.
- Engage with Medicaid planning professionals who can help navigate the complex rules and maximize eligibility.
- Prepare for the application process by gathering necessary documentation, including bank statements, income verification, and medical records, well in advance.
Understanding and planning around Medicaid eligibility can greatly ease the financial burden of nursing home care.





